
By Dave Spiciarich, MedAmorphosis process expert
Utilize PICK charts to identify workflow disrupters for medical practice process problem solving
When things are not going right in a medical practice, such as staff not answering voicemails and emails in a timely fashion, patient complaints about billing or increasing patient no-shows, it can affect staff morale, workflow and ultimately the patient experience.
As a physician-leader or practice manager, you own the responsibility to spot these points of friction before they snowball and cause real problems. Your first inclination may be to examine your staff: the employees’ attitudes, talents and weaknesses. I urge you to initially examine not your people, but your processes.
If one pain point exists for a practice, most likely several do. As such, it’s important to identify all workflow disrupters and strategize a way to approach solving each one.
The first step to process problem solving: a PICK chart to track ROI
I suggest using the PICK chart, an organizing process first developed by Lockheed Martin for process improvement. The acronym, which stands for Possible, Implement, Challenge and Kill, is a tool to categorize ideas based on a rough estimate of return on investment (ROI).
“Possible” means not a top priority, “Implement” identifies priority actions, “Challenge” means not disruptive but to be considered, and “Kill” means don’t worry about it. More on PICK charts in a moment. 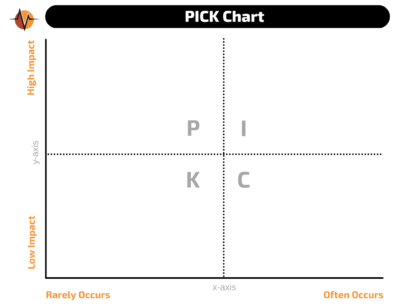
A practice should identify problem areas and document the processes currently in place around each, one at a time. Ideally this would be done together as a team using a whiteboard.
-
- Choose one problem area to discuss.
- Enlist practice staff to identify in their own words the individual steps and the order of the steps in the current way this area is handled.
- Be sure to include staff members in different positions to participate and list their contributions to the process, even if it’s peripheral.
- The more detailed or granular the list of steps, the better.
Let’s look at an example. Vanguard conducted a MedAmorphosis process improvement project for a medical practice that had selected its problem area: patients were complaining about the wait for checking in at appointments. One patient even said she felt like the next patient in line was watching her put in her credit card payment.
Our first step was to validate these complaints, so we asked one of the practice nurses to sit in the waiting area and observe activity for a day. Sure enough, patients would often be stacked four or five deep at the start of the day and at some other times as well. There wasn’t much space in front of the reception desk, so it did get crowded.
Later that day the nurse observed that patients who were trying to set their next appointment were often jammed against patients checking in. The nurse also noted that this was a HIPPA violation, as everyone in line could hear and see others’ check-in and check-out details.
The complaint was not only valid but could cause a larger problem for the practice than just patient satisfaction. (See more about this case study below.)
Play “To Tell the Truth”
When you begin identifying your problem areas, once the current steps have been defined the team can begin exploring the underlying issues. For each step, staff members are invited to identify the problems that they and their patients (and even pieces of information, such as a misplaced paper chart that takes valuable time to hunt down) experience as they move from step to step.
You want to be sure the important issues are revealed, so it’s critical to foster a safe and open environment for this discussion. Follow the rules for effective brainstorming:
- Write down all ideas.
- No one can voice criticism as ideas are revealed.
- All ideas, thoughts and experiences are allowed and documented.
- The collected information will likely be helpful for future process problem solving.
Hopefully, you’ll end up with a pretty big list of issues. While some of the ideas can be tossed out as unimportant or not relevant to the question at hand, there will very likely be too much information for your team to sort and analyze. This is where the PICK chart comes in handy.
This tool aids in focusing the team on what is really important – what is going to make the biggest difference to the practice, staff and your patients. It shows you what you need to be working on and provides a roadmap to continually improve the process after the initial fix.
Next, plot the process
On a big whiteboard, draw a frame for a graph with an x- axis along the bottom and a y-axis rising vertically. On the x-axis, note appropriate increments of frequency: how often does the issue occur? The scale is up to you, but generally frequency is gaged from rarely to often (hourly, daily, weekly – whatever makes sense to you).
Along the y-axis, note increments of impact, or how serious it is when the issue occurs. This will range from mild annoyance at the bottom to severe at the top. It’s up to you to define the severity of impact: it could be manageable, like phone system bottlenecks, or complicated, like a negative patient outcome.
Next, place each issue in its proper spot on the grid. A helpful technique is to write an issue on a sticky note and place it on the grid. This will give you the flexibility to move it as you work through your list.
For each issue, ask the team, “How impactful is this?” The more urgent it is, the higher up it will go. Then look to the x-axis and ask, “How often does the issue occur?”
Having facts helps as you place your issues on the grid. Certain individuals may be very affected by an issue, and they will want to be sure it gets placed at the intersection of “very severe” and “all the time.” I’ve facilitated several of these sessions where staff members feel as though every issue is happening all the time and as such, the practice is broken. I assure them that if that were so, the practice couldn’t function at all.
It’s important to look at the x and y factors dispassionately as you place the issues on the grid. When you’ve gone through all your issues, it’s time to apply the PICK.
PICKing at the processes
Across the center of the grid, draw a vertical and horizontal line. This divides the space into four equal quadrants.
The top left area contains the issues that are very impactful but don’t happen that often. This quadrant gets labeled “P” for possible. Note what issues are here because they are important, but they may not be the top priority because they occur less frequently.
The bottom right area will be labeled “C” for challenge. These issues occur often but aren’t that serious. Still, any interruption to your workflow is disruptive and may need to be examined.
The bottom left quadrant gets a “K” for kill, or kibosh. The issues here have little impact and rarely occur. Your team probably doesn’t need to worry about these.
That leaves the issues in the upper right quadrant. These issues are impactful and occur often. These are serious concerns! Label this area “I” for implement, as these are the issues you’ll want to act on right away.
Case study of a medical practice using a PICK chart
A medical practice hired Vanguard’s MedAmorphosis team to help solve a persistent problem: long patient waits at the front desk for check-in. We enlisted the front desk personnel, two medical doctors, three nurses, a lab tech, even a patient from the practice who volunteered to help.
All the stakeholders were present to brainstorm the issues with the check-in process. We spent an hour talking about the issues surrounding this problem:
-
- Check-in at the front desk takes too long.
- Four to five patients arrive at the same time.
- The front desk person checking in patients also checks them out, takes payments and schedules the next appointment.
- Front desk staff also answers the practice phone.
- Front desk staff also takes the payments.
- The area by the front desk is narrow, forcing arrivals to crowd up. (In COVID-19 pandemic times, this would be doubly problematic!)
- Patients who are already waiting for their appointments sit four feet from the front desk and can hear the conversations there.
Next, we used the PICK chart to prioritize remediation efforts. We looked at each issue and placed a sticky note where it belonged on the PICK grid.
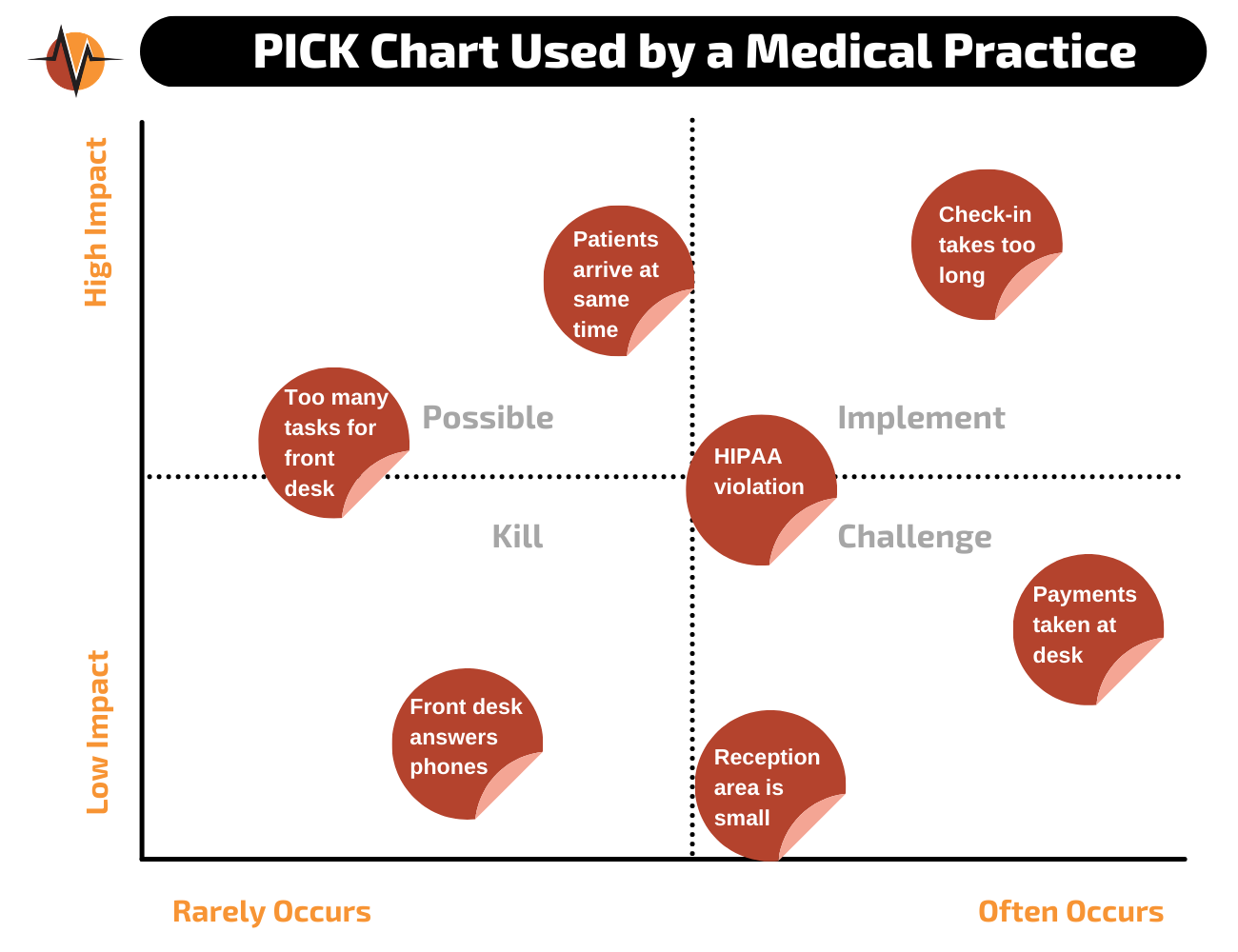
- Check-in takes too long: This happens with every patient and takes about four minutes. If four people arrive at the same time, that’s a 12-minute wait for the last person in line. This kind of waiting happens all the time and is impactful.
- Patients arrive at the same time: This happens when the office first opens and again after it reopens from lunch. Four-to-five appointments are scheduled at the same time, and these patients arrive at the same time. This situation occurs sometimes and is impactful.
- The front desk staff have too many tasks: This is only impactful sometimes, when there is a line of arrivals.
- The front desk staff also answers the phone: The overlap of phones ringing and patients waiting to check in happens sometimes and is annoying.
- Payments are taken at the front desk: This is part of the four-minute check-in. It occurs every time and is somewhat impactful.
- The reception desk area is narrow: Crowding occurs twice a day and is not very impactful.
- Patients can hear other patients’ check-in and check-out details: Occurs often. It’s not very impactful to patients, but potentially could be to the practice financially and legally.
Looking at the PICK chart we see that the check-in process sticky note sits at the top right of the chart, so clearly this problem needs to be solved first. Four minutes seems like a very long time to have someone at the desk. It happens with every patient and leads to many of the other issues.
Let’s look at some of the other issues. The front desk person having to perform numerous activities was something the team decided to consider later. Regarding the check-in area being too narrow, the team determined it was not a very big deal for the practice and it got killed for the time being. Other things were noted for later consideration.
Tips for using the PICK chart in process problem solving
The PICK chart is a great tool for building team morale and getting everyone involved in the practice’s improvement through process problem solving.
Moving from the top right corner toward the center, your process improvement projects can get ranked and hopefully implemented. Be sure to record and save all the issues. Those in the “possible” and “consider” zones are still hurting your performance, and you will need to judge when to tackle these. Once you’ve improved your priority issues, these “considers” will become more of a priority.
As with any improvement tool, this one should be administered with discipline. People are clever, and as soon as they understand PICK, they will maneuver to get their pet project moved into the “implement” area. Watch out for personal agendas and game playing. Anecdotal evidence, while entertaining, can divert your team to a less important issue rather than working on impactful improvements. Rely instead on our friends: facts and data.
I like to think the PICK chart serves two purposes. It helps a practice identify the real problems, then qualify them to start working on the most impactful ones right away. Foundationally, it helps the team see all the issues and how they affect the medical practice culture and morale.
More practice management advice
On The Wired Practice blog, find a wealth of free advice from our on-staff physician and medical process improvement experts on practice management, marketing and more.